Mapping and Ablation of Outflow Tract VT

Raja Selvaraj, JIPMER
Introduction
Outline
- Outflow tract VT - Anatomy
- Outflow tract VT - Mapping tips
- Outflow tract VT - Ablation tips
- Covered in other talks - Summit VT, Safety during VT ablation
Outflow tract VTs - Spectrum of origin
- RVOT (70-80%)
- Below the valve
- Above the valve
- In the cusps
- LVOT (12-45%)
- Aortic sinus of valsalva - LCC, RCC, NCC
- Below the valve
- Superior basal septum
- Aorto-mitral continuity
- LV summit
Anatomy
Outflow tract anatomy
- Understanding of anatomic relationships especially important in this region
- Simplistic models are wrong
Anatomic considerations
- RVOT is anterior and to left of LVOT
- RVOT is a cylinder wrappng around the LVOT
- Pulmonary valve is cephalad and in different plane to aortic valve
- What we call septal rvot is posterior RVOT,
Anatomy - Short axis view as in Echocardiography
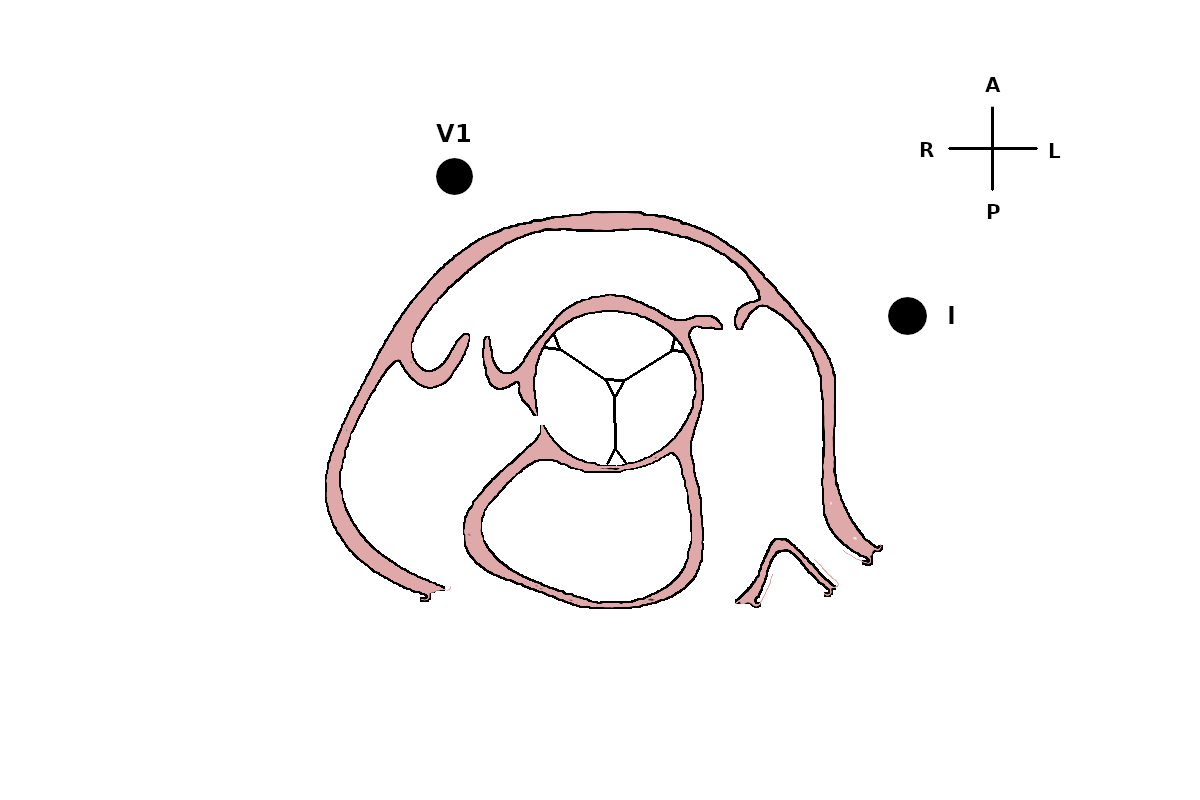
Makes it easier to understand ECG findings
- Lead V1
- Negative for anterior rvot
- Small positive with posterior rvot
- Small positive with origin above pulmonary valve
- Lead I
- Negative above the valve
- Lead avl
- iso / small pos - peri His region
- II/ III ratio
- Higher in III for supravalvar (leftward origin)
Supravalvar Muscle extensions
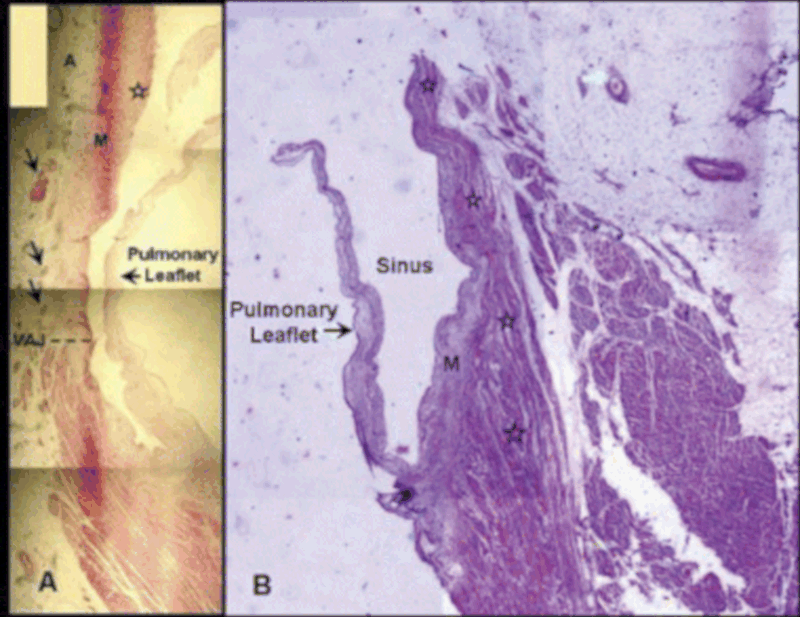
Mapping
ECG localization
- Limb leads to identify outflow tract origin
- Precordial leads to decide chamber to map
- Precordial transition - V3
Growing R wave with more posterior position
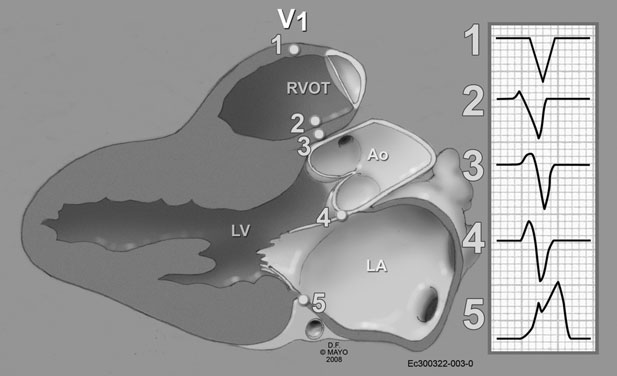
Correlative Anatomy for the Invasive Electrophysiologist: Outflow Tract and Supravalvar Arrhythmia SAMUEL J. ASIRVATHAM, M.D. J Cardiovasc Electrophysiol, Vol. 20, pp. 955-968, August 2009
V3 transition
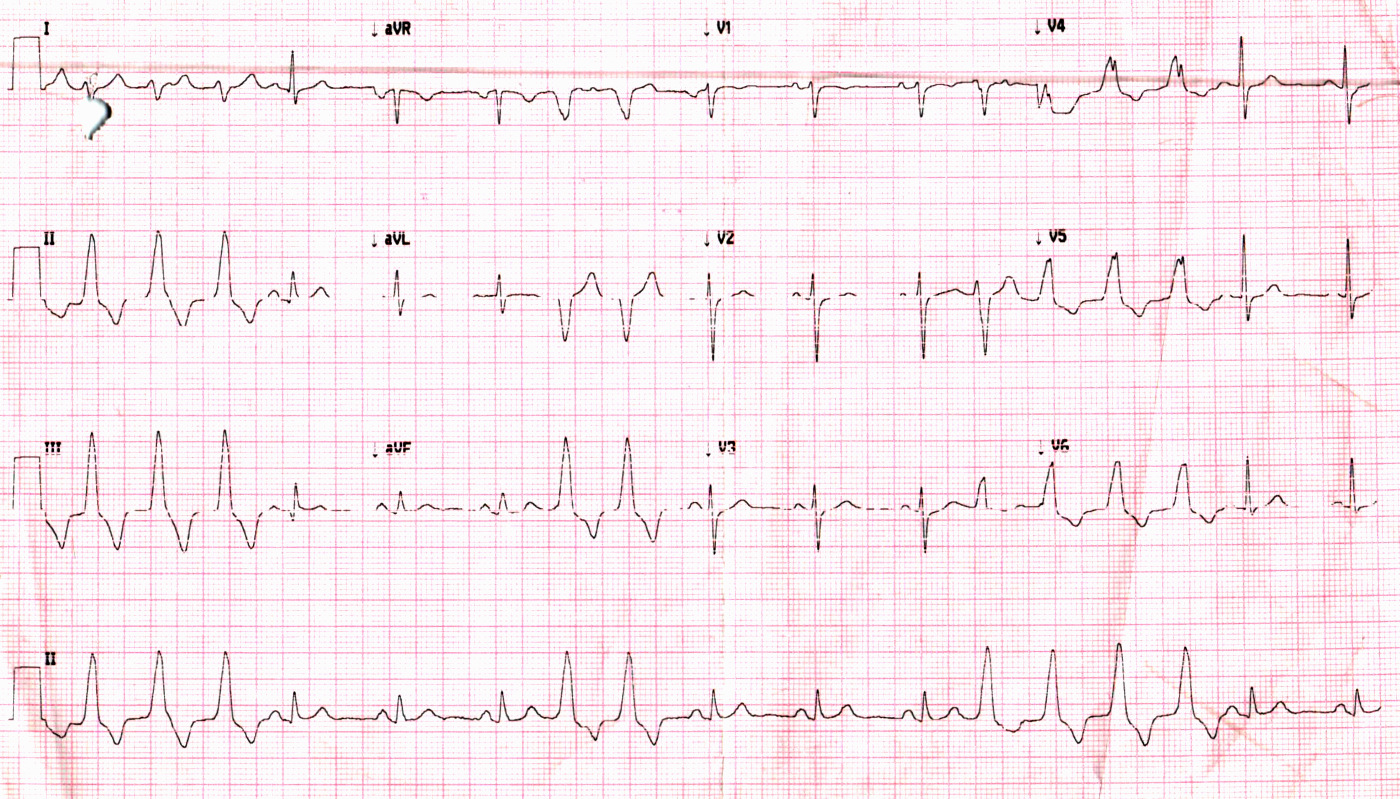
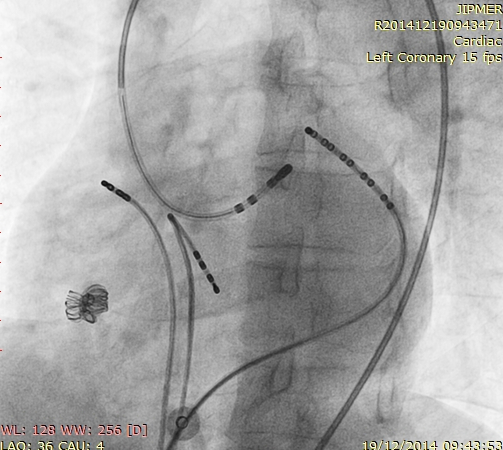
CS catheter
- Almost always useful to have a deeply placed CS catheter
- Triangulation to identify presumptive origin - GCV/AIV junction, LCC and RVOT
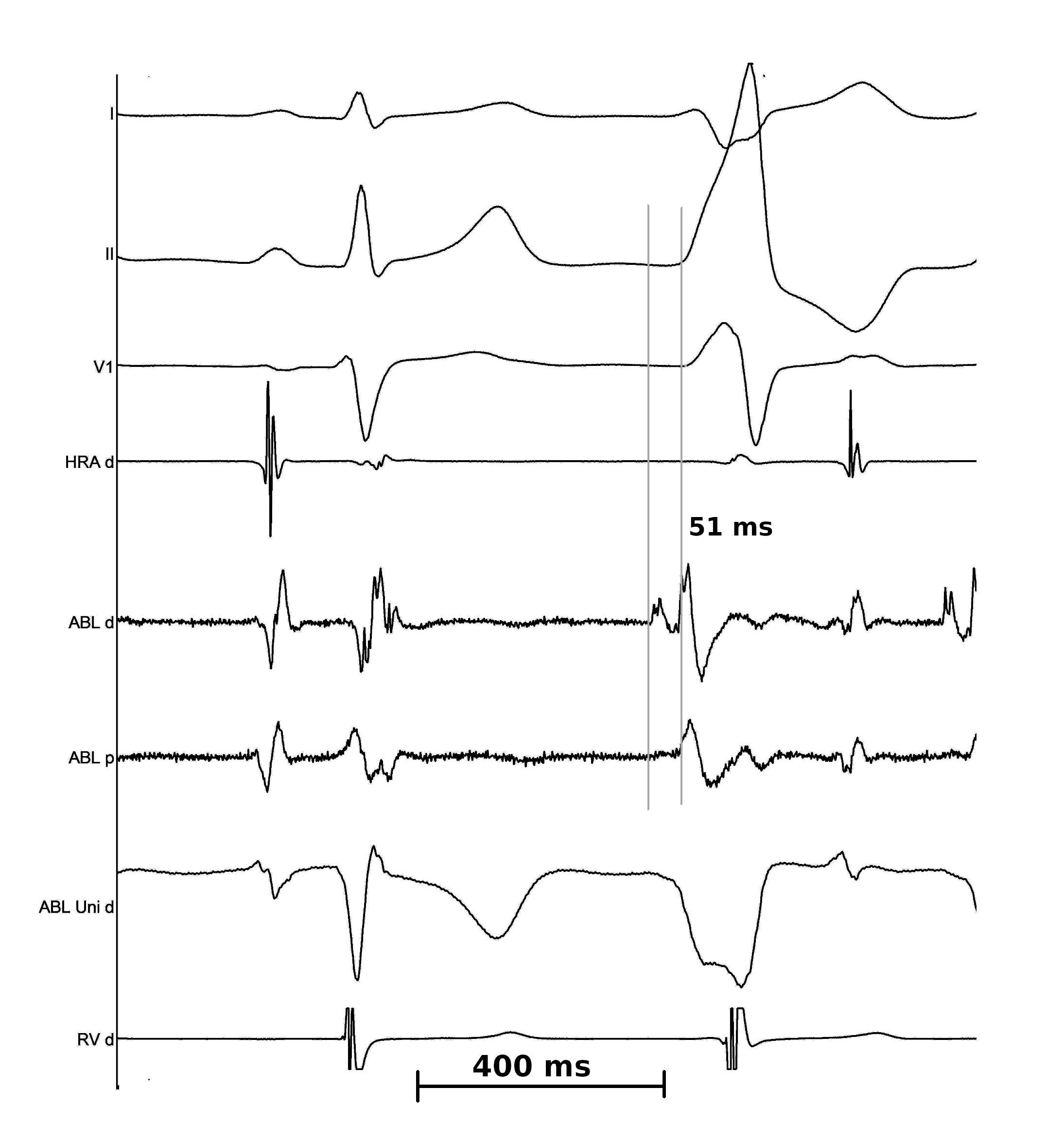
Bipolar EGM
- Timing of near field EGM is key to mapping
- Identify near field / far field
Distinct EGM when mapping above the valve
- Muscle sleeve with fibrous / fatty tissue acting as substrate
- Typically seen above the aortic valve and pulmonary valve
- Late in sinus rhythm and early before PVC
Komandoor S. Srivathsan et al. Mechanisms and Utility of Discrete Great Arterial Potentials in the Ablation of Outflow Tract Ventricular Arrhythmias. Circulation: Arrhythmia and Electrophysiology. 2008;1:30–38
Unipolar EGM
- Concordant with bipolar for RVOT without prior ablation
- May not concur in setting of prior ablation
- May not be useful while mapping above the valve
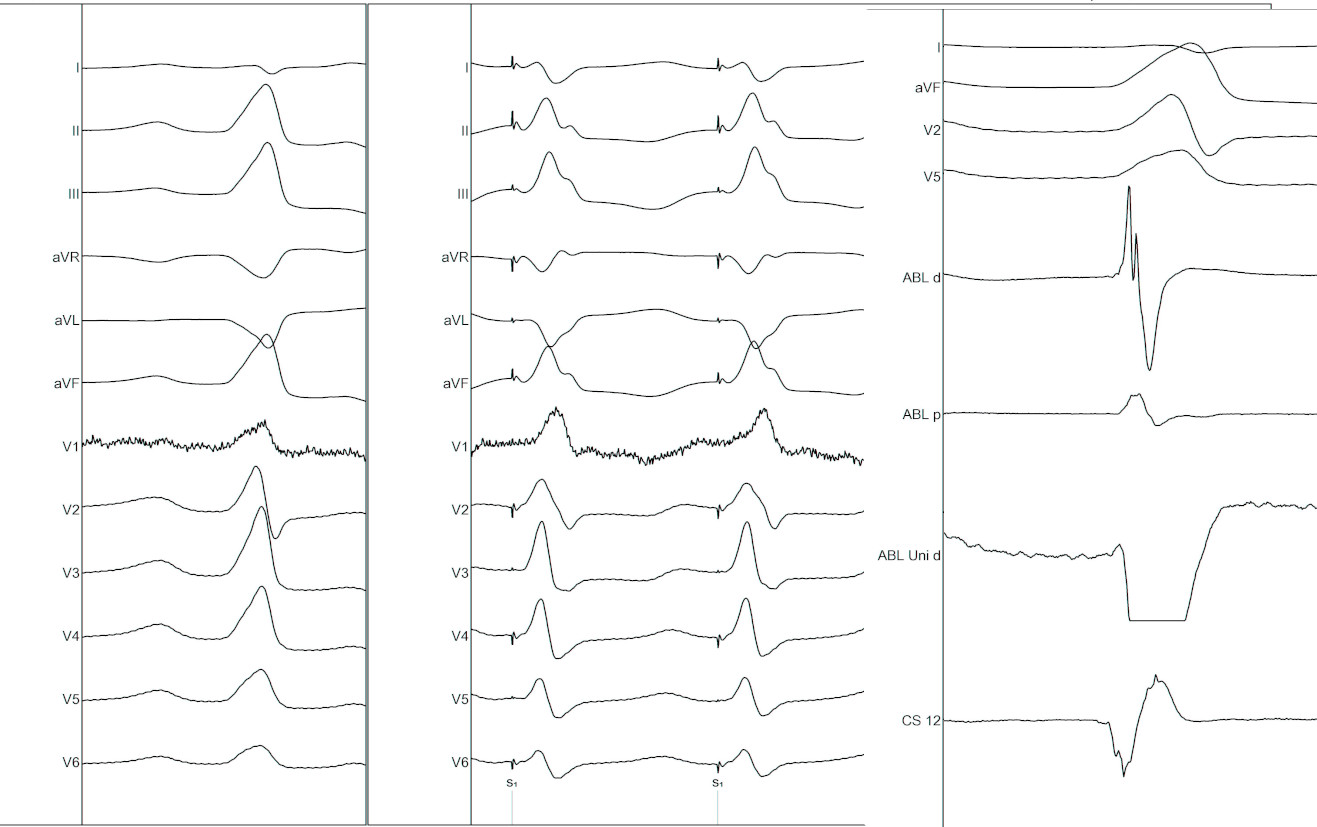
Pace mapping
- Useful as adjunct to activation mapping
- Useful to map faster when PVCs are infrequent
- Lacks specificity
LVOT mapping
GCV mapping
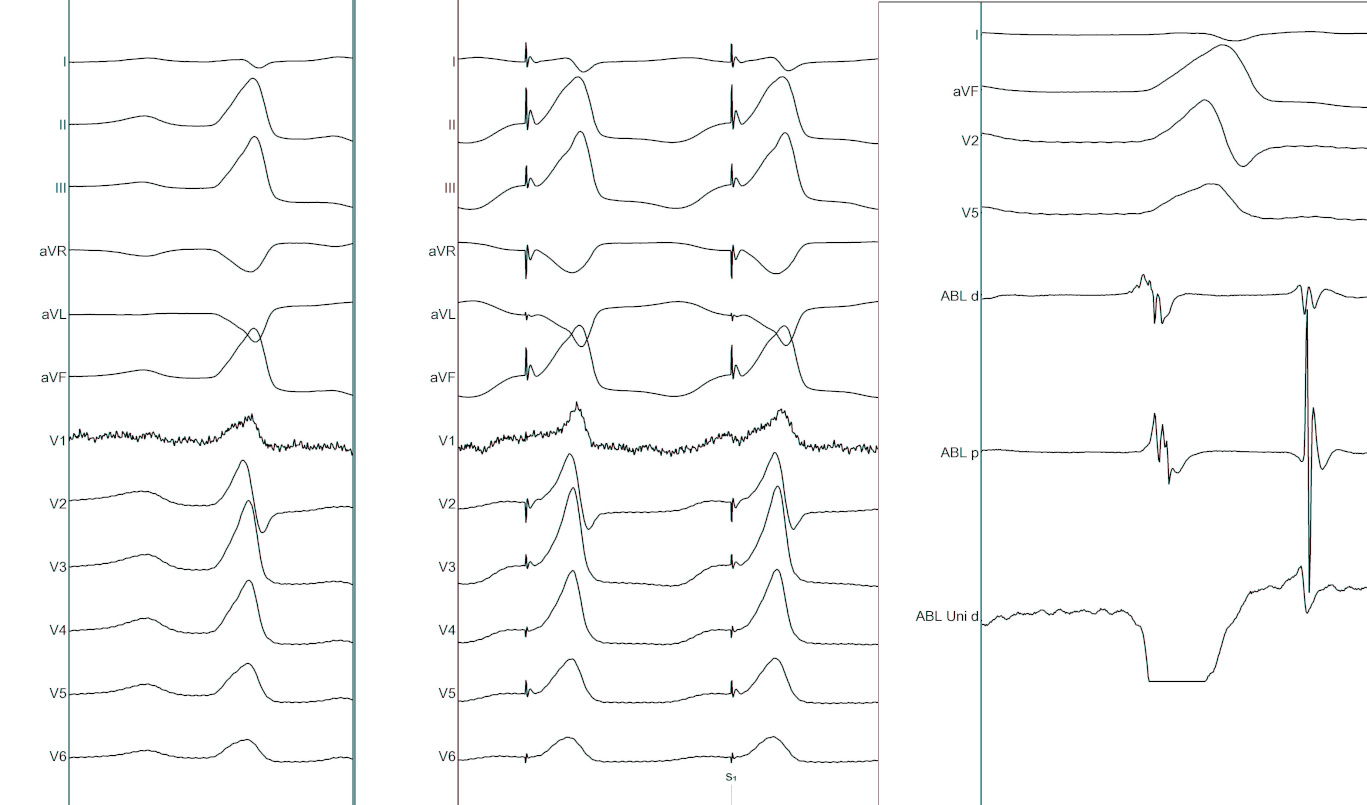
Conflict between pace mapping and activation mapping
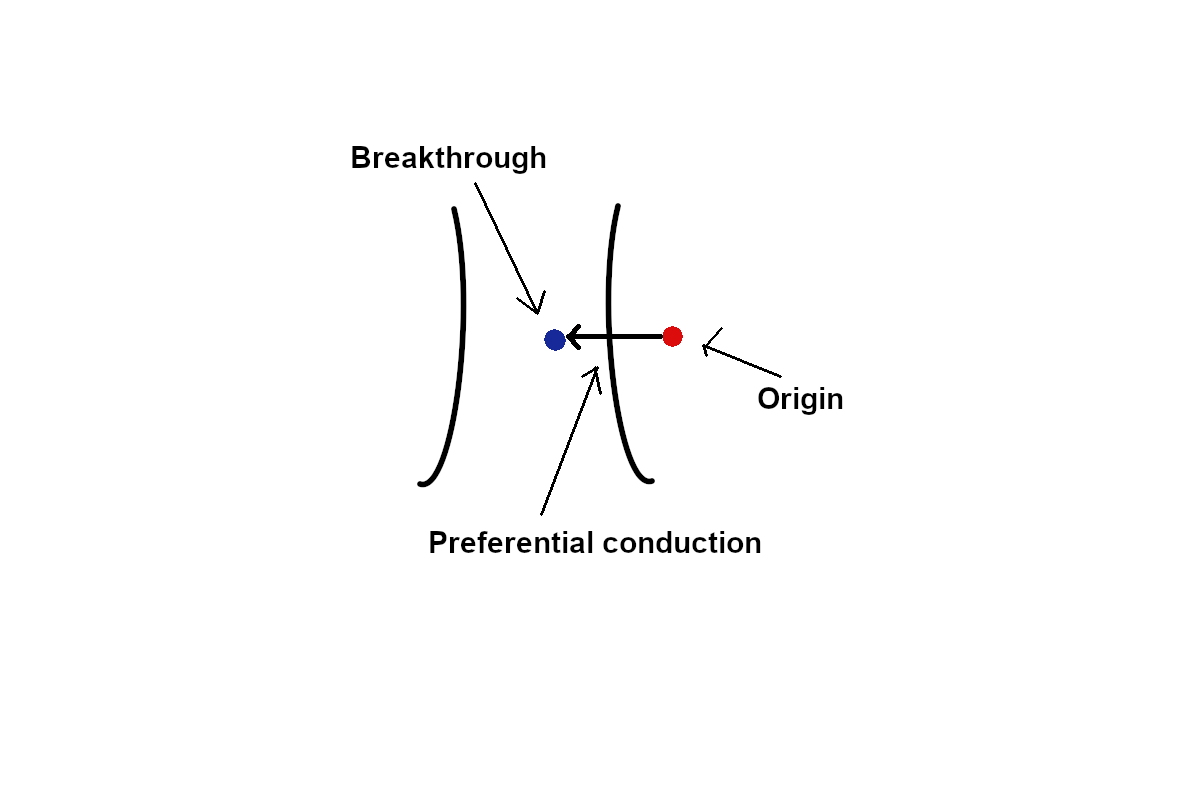
Wavefront spread
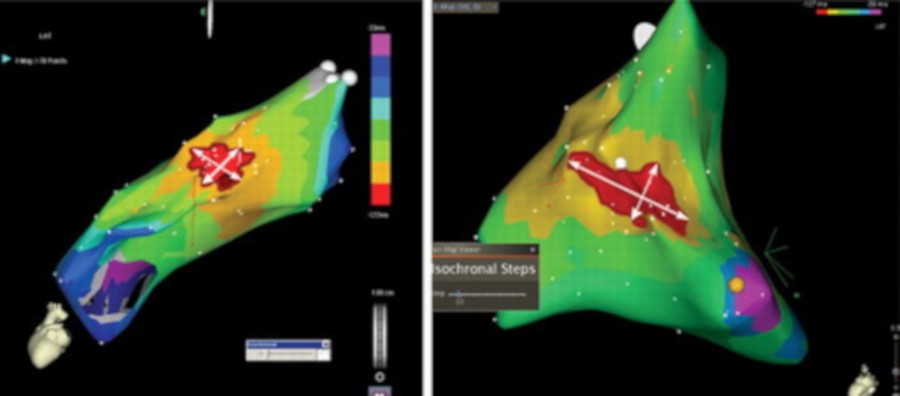
Csaba Herczku … Josep Brugada. Mapping Data Predictors of a Left Ventricular Outflow Tract Origin of Idiopathic Ventricular Tachycardia With V3 Transition and Septal Earliest Activation. Circulation: Arrhythmia and Electrophysiology. 2012;5:484–491
Utility of three dimensional mapping
- Limited incremental value over conventional mapping
- Reduces fluoroscopy time
- Useful in tagging sites and reinforcing lesions
Non contact mapping for unstable VT

Fung JWH, Chan HCK, Sanderson JE. Ablation of haemodynamically unstable right ventricular outflow tract ventricular tachycardia guided by non-contact mapping. Heart 2002;87:15.
Paul AFriedman et al. Noncontact mapping to guide ablation of right ventricular outflow tract tachycardia. JACC 2002;39:1808-1812
Ablation
What catheter ?
- In supravalvar LVOT non-irrigated may be preferred
- LVOT below the valve and RVOT, irrigated may be used
Low powers may be effective in the aortic cusps
- 15-30 W may suffice
- Immediate cessation of PVCs indicator of success
Kabilan … Raja Selvaraj. Low power ablation for left coronary cusp ventricular tachycardia—Efficacy and long-term outcome. Indian Heart Journal 2018;17:S384-S388
Ablation in coronary cusps - Aware of relationship to coronaries
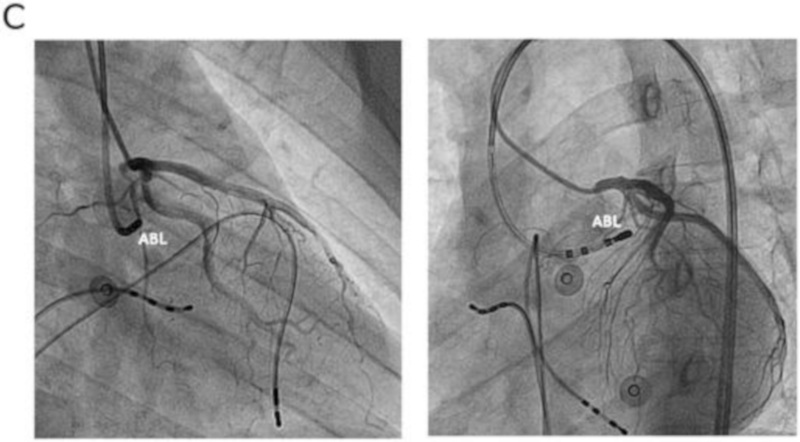
Difficult cases
Supravalvar RVOT VT
- Most from close to pulmonary valve
- Can be above the pulmonary valve level (1)
Timmermans C, Rodriguez LM, Crijns HJ, Moorman AF, Wellens HJ. Idiopathic left bundle-branch block-shaped ventricular tachycardia may originate above the pulmonary valve. Circulation 2003; 108: 1960–1967.
PA origin VT
- Large amplitude R waves in inferior leads
- aVL q > aVR q
Pulmonary sinus cusp VT
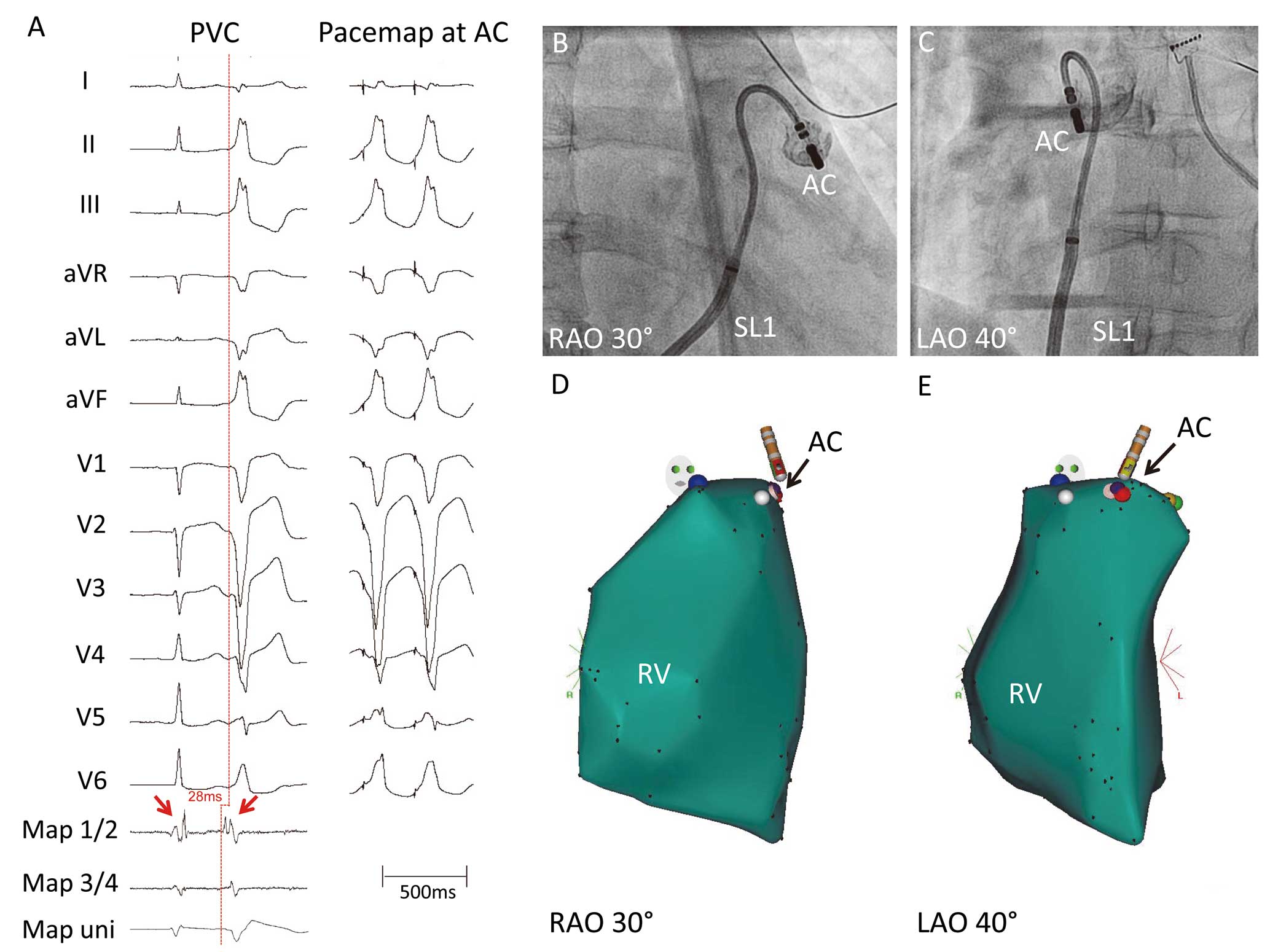
Liao Z, Zhan X, Wu S, Xue Y, Fang X, Liao H, et al. Idiopathic ventricular arrhythmias originating from the pulmonary sinus cusp: Prevalence, electrocardiographic/electrophysiological characteristics, and catheter ablation. J Am Coll Cardiol 2015; 66: 2633–2644.
Intramural foci - Venous branches
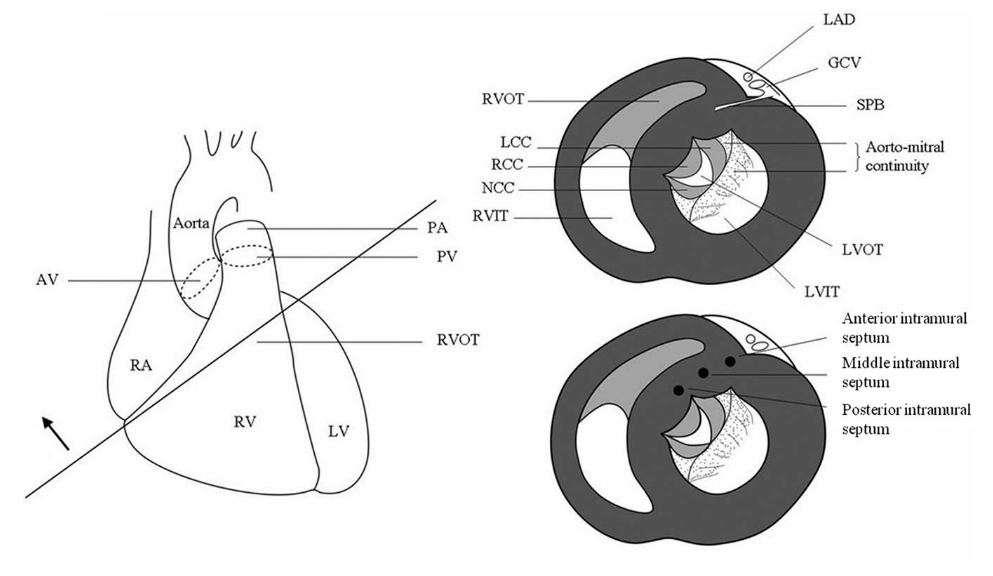
Hongwu Chen et al. Intramural Outflow Tract Ventricular Tachycardia. Anatomy, Mapping, and Ablation. Circ Arrhythm Electrophysiol. 2014;7:978-981.
Intramural foci - Irrigated bipolar ablation
Bipolar ablation from both sides of the septum may sometimes be effective
Teh AW, Reddy VY, Koruth JS, Miller MA, Choudry S, D’Avila A, et al. Bipolar radiofrequency catheter ablation for refractory ventricular outflow tract arrhythmias. J Cardiovasc Electrophysiol 2014; 25: 1093–1099.
Improve contact - Transseptal approach and reverse S curve
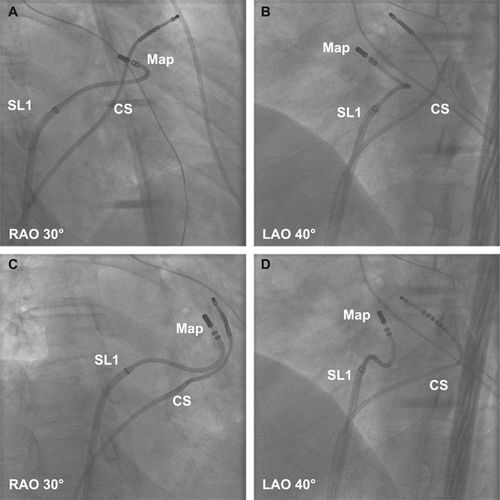
Ouyang F, Mathew S, Wu S, Kamioka M, Metzner A, Xue Y, et al. Ventricular arrhythmias arising from the left ventricular outflow tract below the aortic sinus cusps: Mapping and catheter ablation via transseptal approach and electrocardiographic characteristics. Circ Arrhythm Electrophysiol 2014; 7: 445–455.