
Ventricular arrhythmias after myocardial infarction - Management
Raja Selvaraj
Cardiac Electrophysiologist
Professor of Cardiology
JIPMER
Scenario 1 - NSVT / PVCs late after MI
Case 1
- 64 year old male
- Old IWMI, LVEF 40%
- Frequent PVCs - RBBB / LAD
- Mild DOE class II
Does it need to be treated, and if so why ?
Possible indications to treat
- To reduce risk of sudden death
- To improve symptoms
- To improve EF
Sudden death
- NSVT / PVCs after MI indicate higher risk
- However, treating them does not alter risk
Other reasons to treat
- Symptomatic - need to treat
- To improve EF ?
Can it be a cause of arrhythmia induced cardiomyopathy
- Frequent PVCs can cause AICM
- AICM can also occur in setting of underlying structural heart disease
- Based on PVC load in Holter and Echo findings, RFA done
Does it need ICD implant ?
- Secondary prevention indication only for sustained VA
- Primary prevention indication only when EF less than 30% / 35%
- With EF > 40, no evidence that NSVT / PVCs indicate need for ICD
Management
- Symptoms only effort intolerance
- Holter - 24% PVCs
- Fall in LVEF
- Underwent successful ablation
- Improvement in EF during follow up
Summary
- Non sustained VT / PVCs marker can be marker of higher risk after MI
- Not significant without severe LV dysfunction
- Treatment with AAD does not alter survival
- Treatment may be required for symptoms or to improve LV function
Scenario 2 - Sustained VT late after MI
Case 2
- 35 year old male
- CAD - AWMI 1 year back
- CAG - showed non obstructive LAD disease
- LVEF 38 %
- Presented with palpitations
ECG
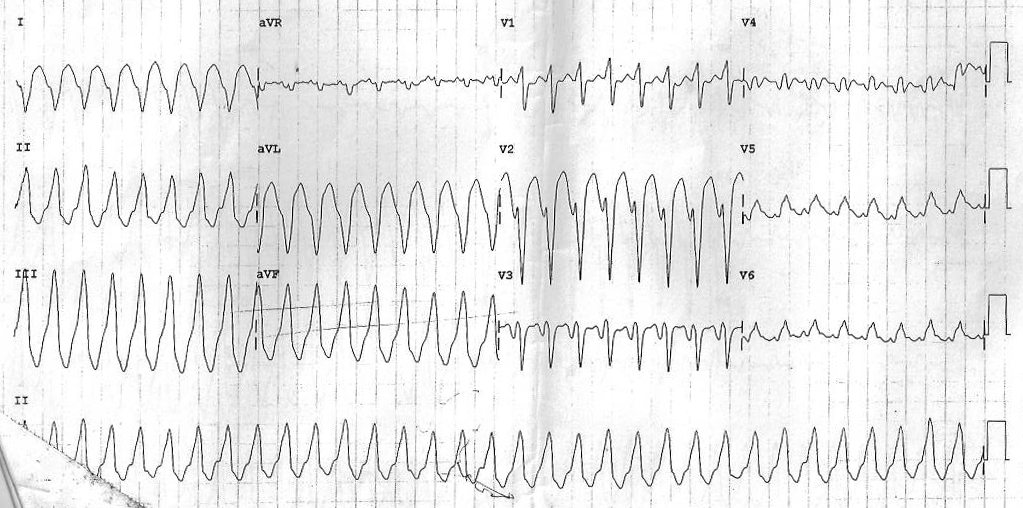
ECG after cardioversion
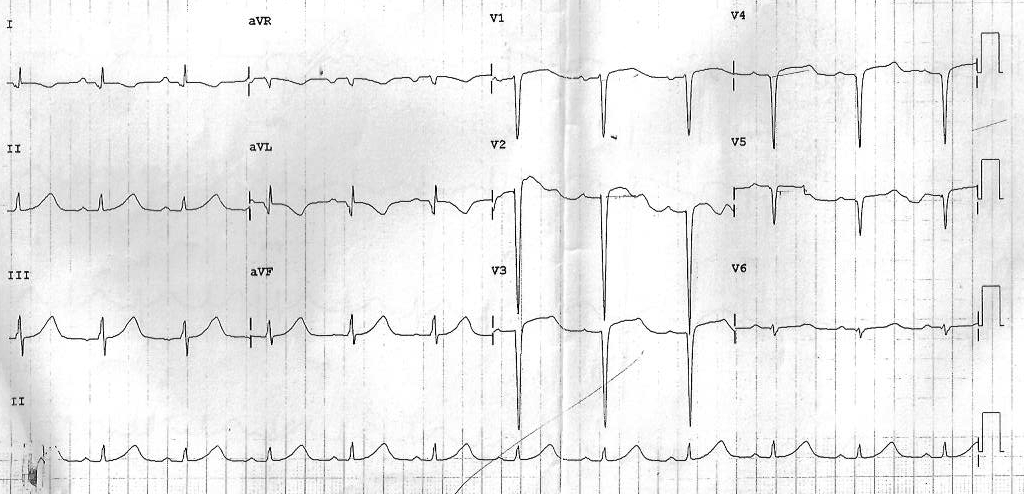
Does he need CAG and revascularization ?
- A. Yes
- B. No
CAG and revascularization
- Polymorphic VT / VF can be due to reversible ischemia
- Sustained monomorphic VT not due to ischemia
- Modest elevation of biomarkers does not indicate ischemia
- Re test after 3 months if possibly reversible after revascularization
Does he need ICD implant ?
- A. Yes
- B. No
ICD for secondary prevention
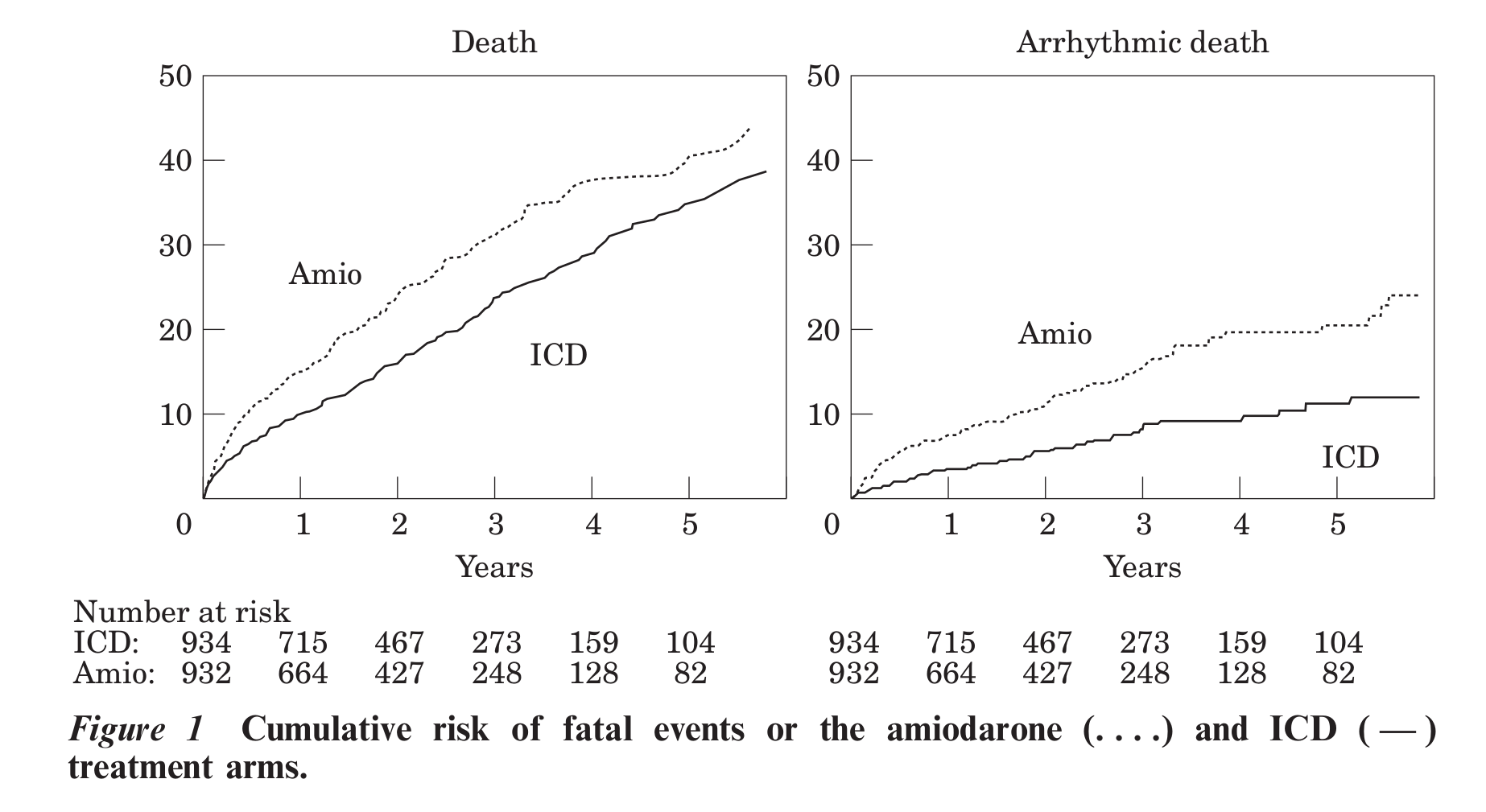
S. J. Connolly, A. P. Hallstrom, R. Cappato, E. B. Schron, K.-H. Kuck, D. P. Zipes, H. L. Greene, S. Boczor, M. Domanski, D. Follmann, M. Gent, R. S. Roberts, investigators of the AVID, CASH and CIDS studies, Meta-analysis of the implantable cardioverter defibrillator secondary prevention trials, European Heart Journal, Volume 21, Issue 24, 1 December 2000, Pages 2071–2078, https://doi.org/10.1053/euhj.2000.2476
What ICD will you implant
- A. Single chamber
- B. Dual chamber
When to use a dual chamber ICD
- Indication for pacing
- Possible future need for pacing
- Does not reduce inappropriate therapies
What ICD lead ?
- A. Single coil
- B. Dual coil
Single coil lead
- Higher DFT
- Sufficient for most patients
- Easier to extract in long term
After ICD implant
- A. Continue Amiodarone
- B. Stop Amiodarone
Anti-arrhythmic drugs
- ICD does not prevent VT
- ICD is not a treament for VT
- Amiodarone reduces recurrences, low proarrhythmic risk
- But amiodarone doesn't save lives
When would you advise ablation ?
- A. Upfront along with ICD
- B. If recurrence on amiodarone
- C. Increase dose of Amio / add Mexilitene on recurrence, then ablation if recurrence again
Upfront ablation

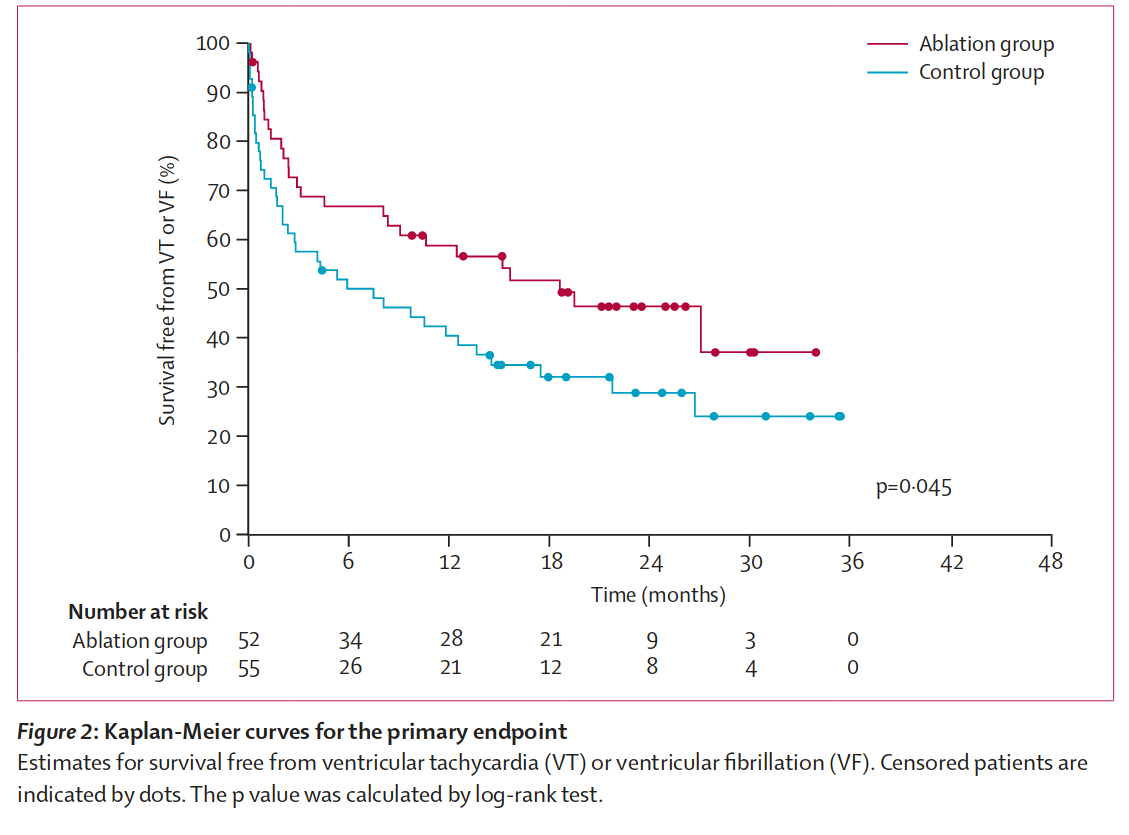
Ablation or drug escalation ?

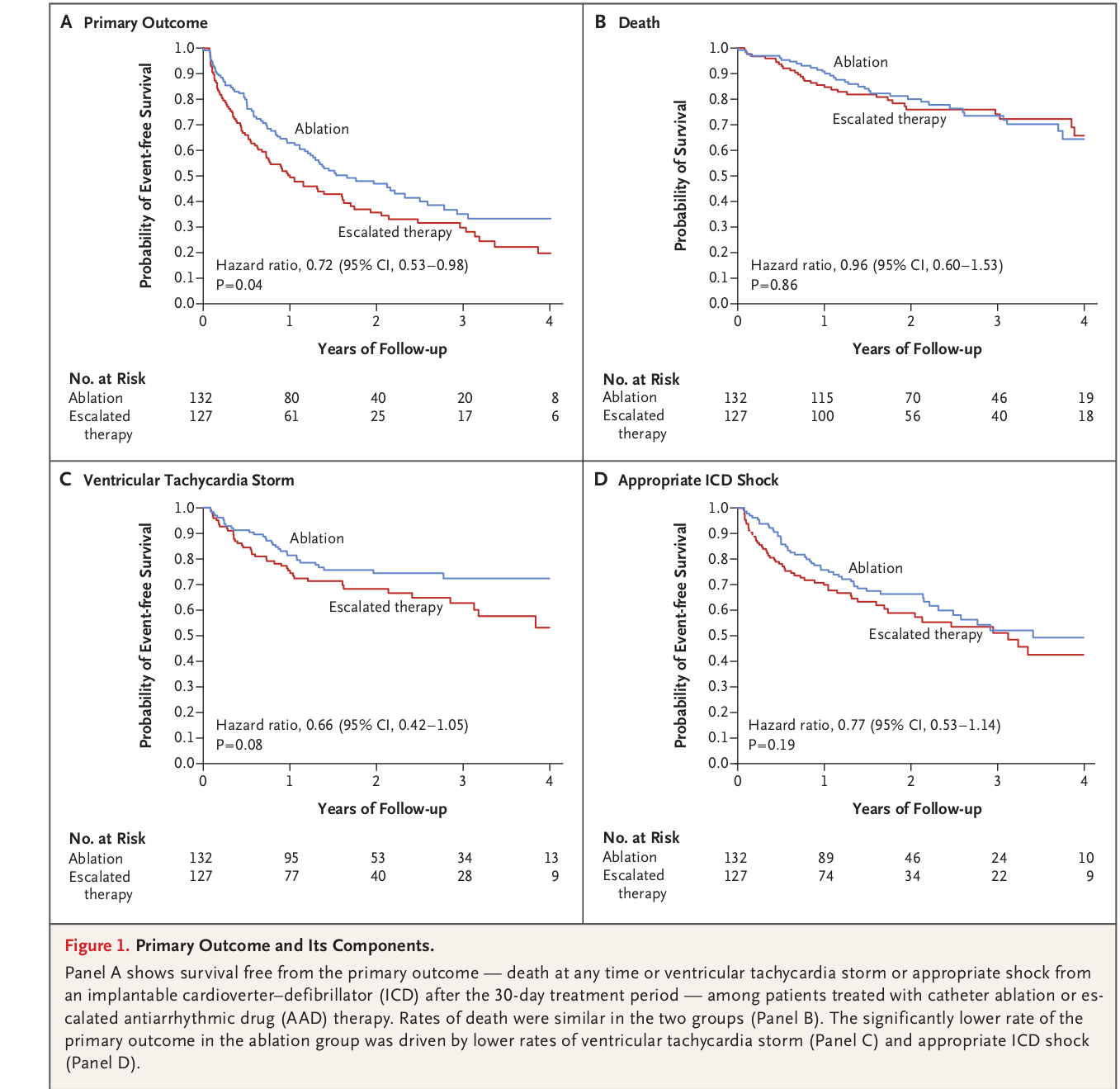
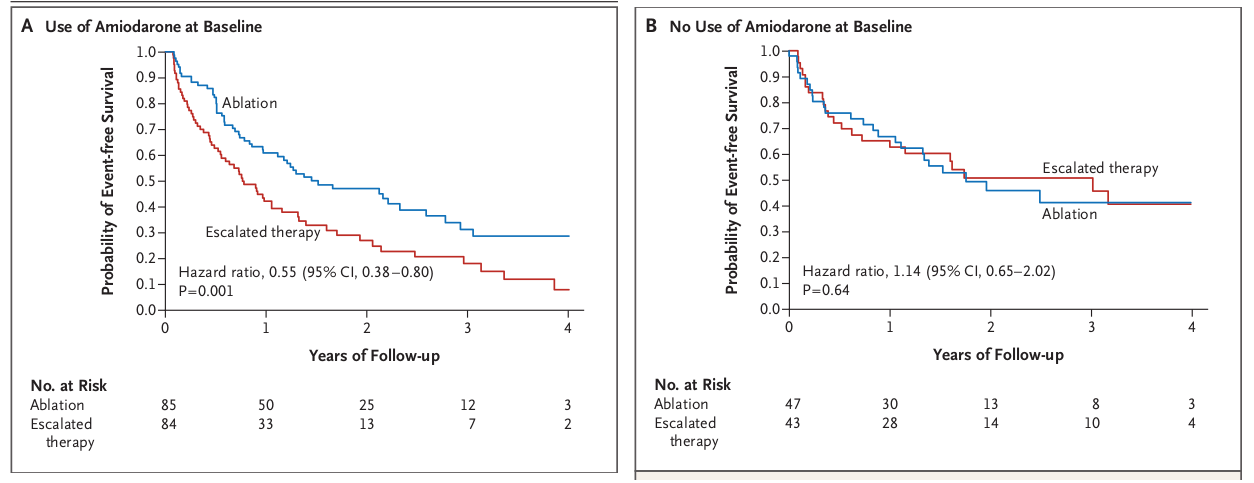
Management
- Treated with amiodarone 200 OD and beta blocker
- Single chamber ICD implanted
- Recurrence of VT 2 years afterwards
- Underwent RFA and withdrawal of Amiodarone after 6 months
Summary
- Sustained VT after MI indicates high risk of SCD and need for ICD implant
- AAD or ablation required to prevent VT
- AAD as first choice followed by ablation on drug failure is reasonable
- Ablation as first line may also be considered