
Wearable Devices in Cardiovascular Medicine - When and how to use them.
Raja Selvaraj
Professor of Cardiology
JIPMER
Introduction
What are "wearable devices" in the context of medicine ?
- Digital medicine tools
- Process data captured by mobile sensors
- Generate measures of behavioral or physiological function
- eg. Physical activity (PA), heart rate (HR), heart rhythm, and sleep
Not just in realm of fiction anymore

Devices
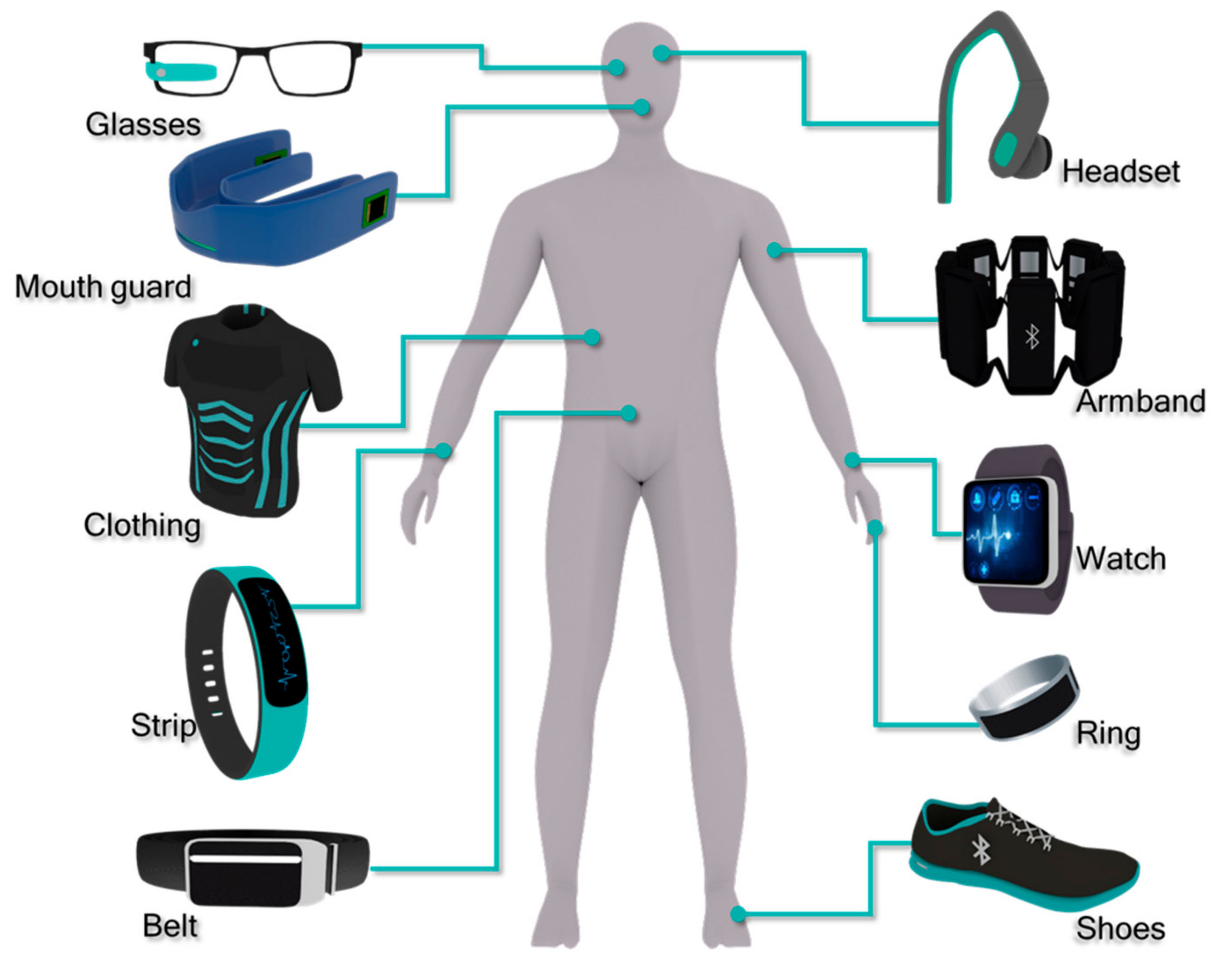
Types
- Consumer grade
- Medical grade
- Research grade
Sensors
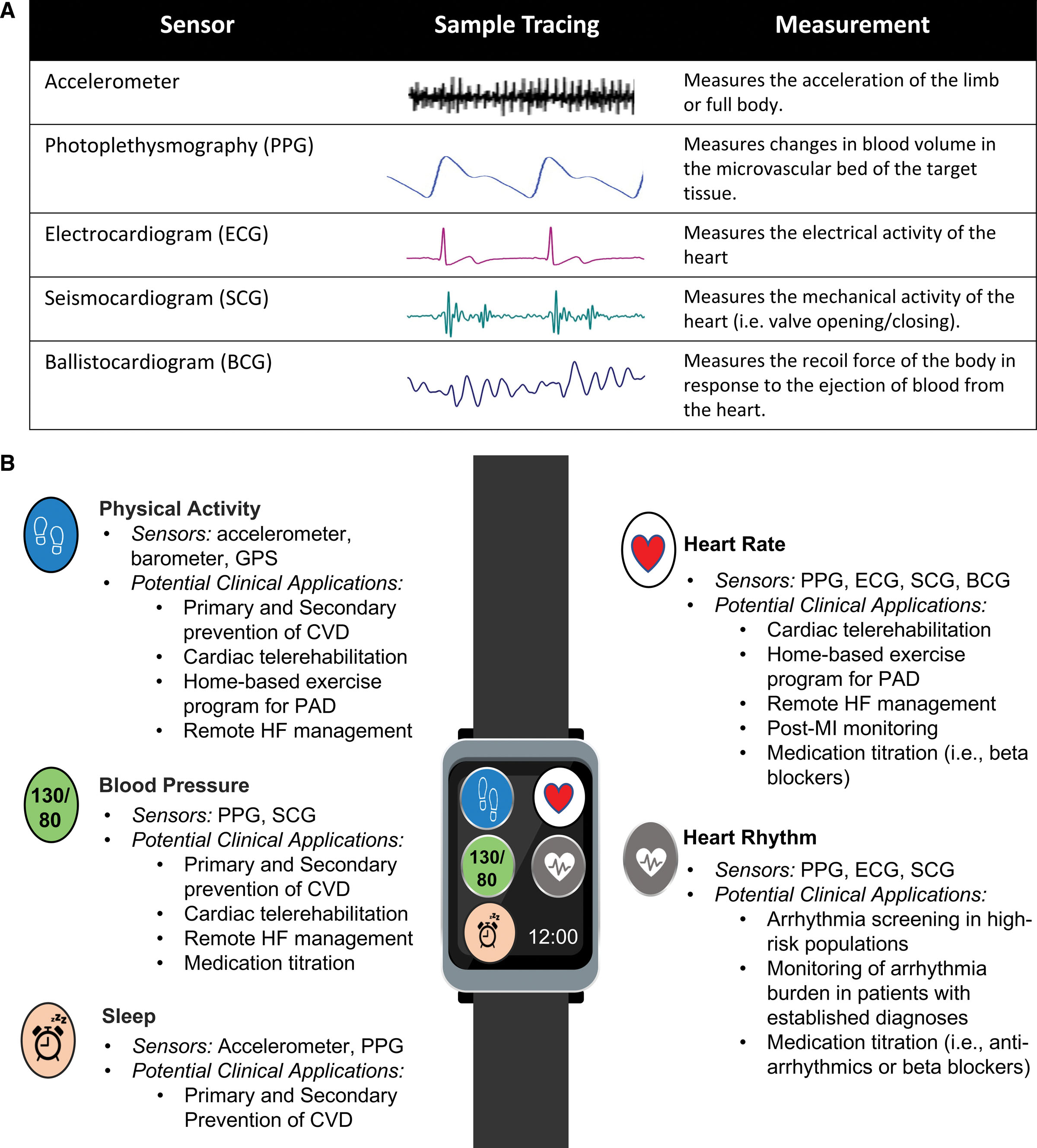
Sensors
- Accelerometer
- microelectromechanical system sensors that measure the acceleration
- Measure volume and intensity of PA
- Photoplethysmogram
- optical measurement of the changes in blood volume in the microvascular tissue bed
- track HR, heart rhythm, and pulse oximetry
- may be useful for blood pressure and vascular aging
- Electrocardiogram
- difference in electrical potential between various points on the body with skin-mounted electrodes
- to monitor HR, detect arrhythmias, and identify myocardial ischemia or infarction
Sensors
- Seismocardiogram
- local vibration of the chest wall that occurs with every cardiac cycle
- estimate cardiac time intervals, estimate changes in hemodynamics, and characterize whether patients with HF are compensated or decompensated.
- Ballistocardiogram
- recoil forces of the body in response to the cardiac ejection of blood
- estimate HR and assess the clinical state of patients with HF.
Sensors
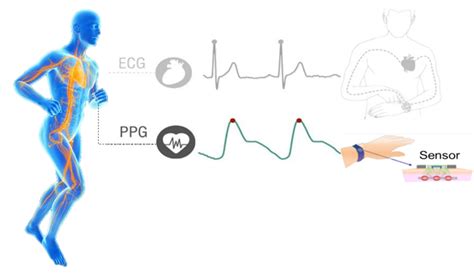
Traditional Machine learning and Deep Learning algorithms
- Reduce noise in data
- Extract information from higher dimensional data
- Representational learning
- On device algorithms / cloud based analysis
Applications
Step count and mortality risk
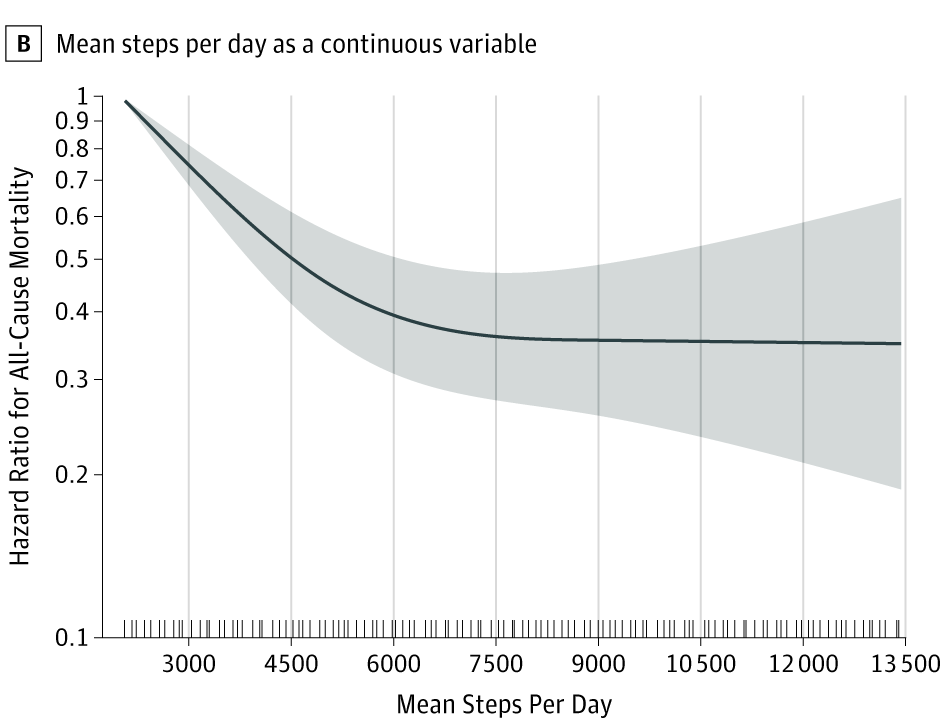
Lee IM, Shiroma EJ, Kamada M, Bassett DR, Matthews CE, Buring JE. Association of Step Volume and Intensity With All-Cause Mortality in Older Women. JAMA Intern Med. 2019 Aug 1;179(8):1105-1112. doi: 10.1001/jamainternmed.2019.0899
Wearables increase physical activity
- On average increase steps by 1800 / day
- Increase walking time by 40 min / day
- Reduce weight by 1 kg
Ferguson T, Olds T, Curtis R, Blake H, Crozier AJ, Dankiw K, Dumuid D, Kasai D, O'Connor E, Virgara R, Maher C. Effectiveness of wearable activity trackers to increase physical activity and improve health: a systematic review of systematic reviews and meta-analyses. Lancet Digit Health. 2022 Aug;4(8):e615-e626. doi: 10.1016/S2589-7500(22)00111-X. PMID: 35868813.
Arrhythmia detection - AF
- Atrial fibrillation may be asymptomatic / minimally symptomatic
- Increases risk of stroke
- Prophylactic anticoagulation in patients with AF at risk of stroke can reduce incidence
- Traditional screening methods are cumbersome
AF detection by smartwatch - Apple Heart Study
- 419,297 participants (siteless study design)
- Median 117 days of monitoring
- 2161 (0.52%) - notification of irregular pulse
- 450 wore ECG patch for 7 days - AF confirmed in 34%
- Positive predictive value of individual tachogram - 0.71
Perez MV, Mahaffey KW, Hedlin H, Rumsfeld JS, Garcia A, Ferris T, Balasubramanian V, Russo AM, Rajmane A, Cheung L, Hung G, Lee J, Kowey P, Talati N, Nag D, Gummidipundi SE, Beatty A, Hills MT, Desai S, Granger CB, Desai M, Turakhia MP; Apple Heart Study Investigators. Large-Scale Assessment of a Smartwatch to Identify Atrial Fibrillation. N Engl J Med. 2019 Nov 14;381(20):1909-1917. doi: 10.1056/NEJMoa1901183. PMID: 31722151; PMCID: PMC8112605.
The Apple Heart Study
- One of the largest studies
- Skewed population - Young, wealthy and healthy
- Only 6% of patients were over 65 yrs
- Low event rate - 0.5% got alerts
- Poor follow up - only 20% got ECG patch
- Positive predictive value - 34%
- Under 40 years - 18%
Wearables for AF screening - Simulation model
- Simulated 30 million person cohort based on US population
- 65 or older with elevated stroke risk (CHADS-VaSc)
- Strategy of wrist worn PPG monitor followed by patch ECG confirmation cost effective
Chen W, Khurshid S, Singer DE, Atlas SJ, Ashburner JM, Ellinor PT, McManus DD, Lubitz SA, Chhatwal J. Cost-effectiveness of Screening for Atrial Fibrillation Using Wearable Devices. JAMA Health Forum. 2022 Aug 5;3(8):e222419. doi: 10.1001/jamahealthforum.2022.2419. PMID: 36003419; PMCID: PMC9356321.
Cardiac tele rehabilitation
- As effective as traditional center-based cardiac rehabilitation
- More cost effective
Brouwers RWM, van der Poort EKJ, Kemps HMC, van den Akker-van Marle ME, Kraal JJ. Cost-effectiveness of Cardiac Telerehabilitation With Relapse Prevention for the Treatment of Patients With Coronary Artery Disease in the Netherlands. JAMA Netw Open. 2021 Dec 1;4(12):e2136652. doi: 10.1001/jamanetworkopen.2021.36652. Erratum in: JAMA Netw Open. 2022 Jan 4;5(1):e2147432. doi: 10.1001/jamanetworkopen.2021.47432. PMID: 34854907; PMCID: PMC8640894.
Who is it for ?
Individuals / Patients
- Promotion of healthy lifestyle choices
- Screening and earlier detection of disease
- Continuous monitoring for safety
- Active role in monitoring and managing chronic conditions
- Telemonitoring - reducing office visits
Healthcare providers
- Improved screening and management of cardiac conditions
- Earlier detection of clinical decompensation
- Assessment of patient adherence
- Additional data for telemedicine visits
Individuals / Patients - Challenges
- Difficulty using technology
- Difficulty due to cognitive, hearing or visual impairment
- Difficulty understanding clinical significance of measurements
- Cost / internet access
- Data security
- Downsides of reduced in-person interaction - Social isolation
- Lack of cultural / language diverse resources
Healthcare providers - Challenges
- Clinical infrastructure and staff to handle data
- Integration of wearables data into EHR
- Lack of standarized reimbursement
- Need for use criteria and guidelines
- Poorly defined regulatory oversight
- Device accuracy and validity concerns
- Data privacy and medicolegal concerns
- Potential new health disparity (digital divide)
Digital divide and healthcare utilization
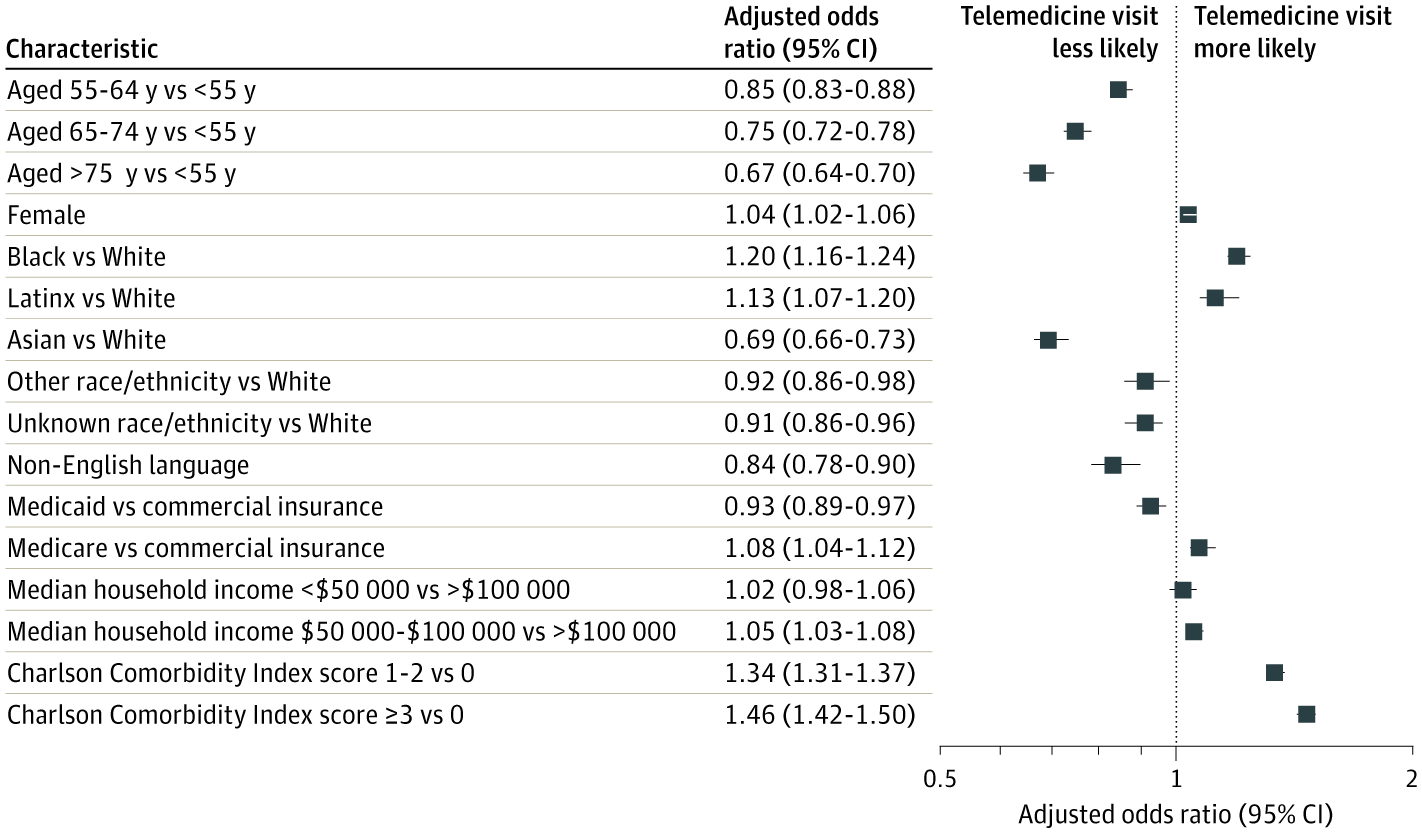
Eberly LA et al. Patient Characteristics Associated With Telemedicine Access for Primary and Specialty Ambulatory Care During the COVID-19 Pandemic. JAMA Netw Open. 2020 Dec 1;3(12):e2031640. doi: 10.1001/jamanetworkopen.2020.31640.
FAIR guiding principles for scientific data management
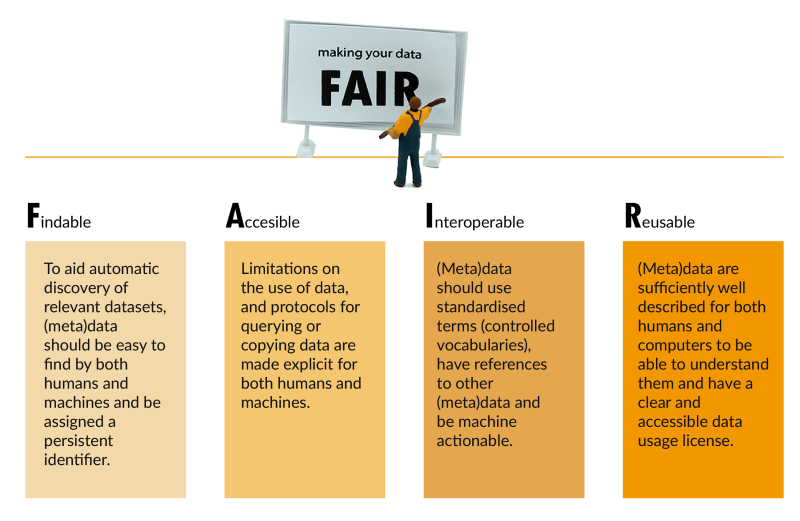
Wilkinson MD et al. The FAIR Guiding Principles for scientific data management and stewardship. Sci Data. 2016 Mar 15;3:160018. doi: 10.1038/sdata.2016.18. Erratum in: Sci Data. 2019 Mar 19;6(1):6. doi: 10.1038/s41597-019-0009-6. PMID: 26978244; PMCID: PMC4792175.
Vision for the future
- Single wearable device with multiple sensors
- Validated / approved algorithms
- Data that is accessible and interoperable
- Connects automatically to EHR
- Data from wearable supplements / replaces in clinic evaluation and monitoring